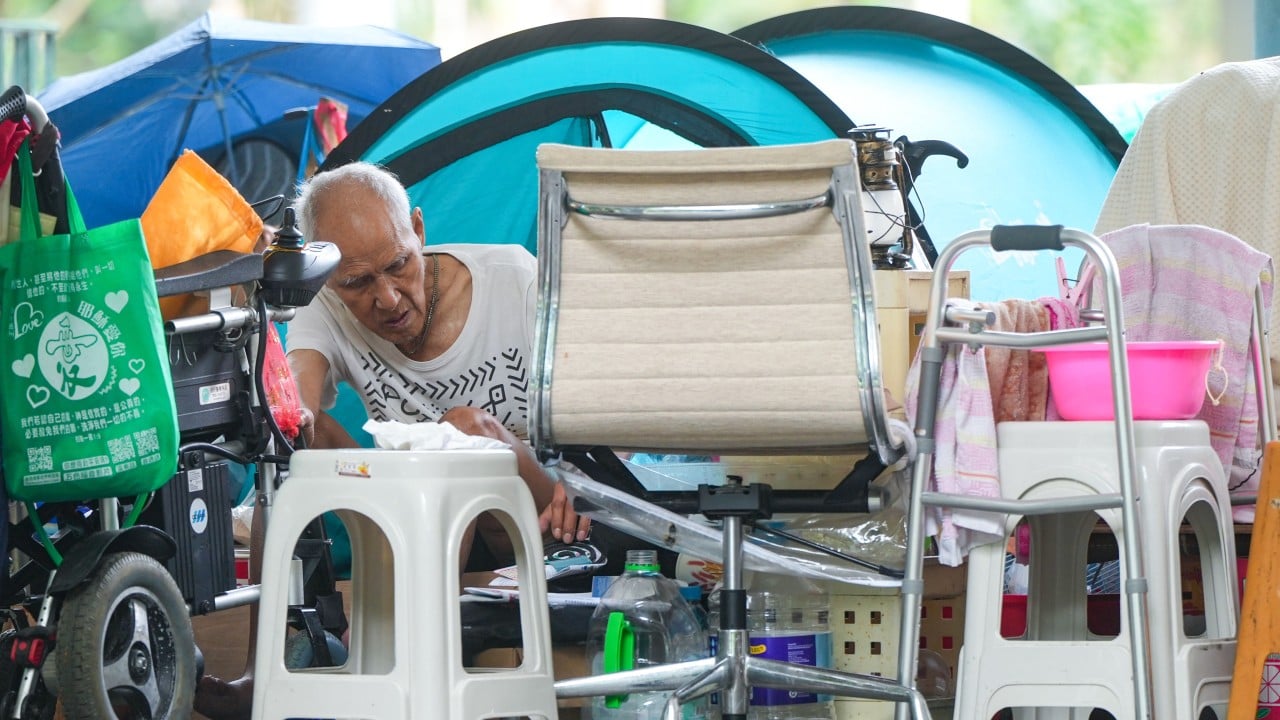
The recent 10% to 20% increase in public medical fees in Hong Kong serves as a stress test for the city's most vulnerable demographic, revealing a critical breaking point in the healthcare safety net. When the baseline for a "plan to reduce medical visits" reaches 60% among the homeless population, the issue shifts from simple affordability to a fundamental breakdown in the social contract. This trend suggests that for individuals living on the periphery of the economy, healthcare has transitioned from a basic right to an elastic luxury good—a shift that inevitably leads to higher downstream costs for the state through emergency interventions and long-term disability care.
The Cost Threshold and Behavioral Modification
Healthcare utilization among the homeless is governed by a strict hierarchy of needs where immediate survival—sustenance and physical security—supersedes preventative or chronic disease management. The decision to skip a medical appointment is rarely a choice of convenience; it is a calculated trade-off within a zero-sum financial ecosystem.
The Marginal Propensity to Forego Care
The "60% threshold" identified in recent surveys indicates a high degree of price sensitivity. In standard economic terms, the demand for healthcare is typically inelastic—people need it regardless of price. However, for the homeless in Hong Kong, this demand becomes hyper-elastic. Because their discretionary income is non-existent, even a marginal increase in the cost of a clinic visit or a prescription co-payment forces a redirection of funds toward immediate caloric intake.
- The Flat-Fee Barrier: While the absolute dollar increase may appear nominal to a middle-class observer, it represents a significant percentage of a street sleeper’s daily liquidity.
- Administrative Friction: Beyond the direct cost, the complexity of fee waiver applications acts as a non-monetary tax. The requirement for proof of address or consistent identity documentation often precludes the very people who need the waivers most.
Structural Determinants of Health Decay
The decline in medical visits is not an isolated metric but a catalyst for a compounding cycle of physical and economic decay. To analyze this, we must look at the three primary channels through which fee hikes accelerate health deterioration.
1. Chronic Disease Mismanagement
A significant portion of the homeless population suffers from "silent" killers such as hypertension and Type 2 diabetes. These conditions require consistent monitoring and medication adherence.
- The Maintenance Gap: When 60% of this group plans to cut visits, the first casualties are the routine check-ups. Missing these leads to unmonitored blood pressure and fluctuating glucose levels.
- The Complication Pipeline: Untreated hypertension leads to strokes; unmanaged diabetes leads to neuropathy and amputations. By saving pennies on primary care, the system guarantees a future expenditure of thousands on surgical interventions and intensive care units.
2. Mental Health and Substance De-escalation
The intersection of homelessness and mental health is well-documented. Public clinics often serve as the only point of contact for psychiatric medication and counseling.
- Relapse Triggers: Financial barriers to psychiatric follow-ups increase the likelihood of medication non-compliance. This frequently results in acute psychotic episodes or a return to substance abuse as a form of self-medication for untreated trauma or anxiety.
- Social Displacement: As mental health stabilizes or declines based on healthcare access, the individual's ability to engage with re-housing programs or employment assistance disappears, cementing their status as "chronically homeless."
3. Communicable Disease Reservoirs
Living in high-density, unsanitary conditions makes the homeless population a primary risk group for communicable diseases, including tuberculosis and respiratory infections.
- The Detection Delay: Reducing medical visits means symptoms are ignored until they become debilitating.
- Public Health Risk: This delay increases the window of time during which an individual can transmit infections to the broader public, particularly in high-traffic areas or public transport hubs where street sleepers often congregate.
The Institutional Failure of the Safety Net
The existence of a fee waiver system suggests, on paper, that no one is denied care. However, the operational reality reveals a disconnect between policy design and human behavior.
Documentation Requirements as an Exclusionary Tool
Hong Kong’s bureaucracy is built on the assumption of a stable domicile.
- Proof of Identity: Many homeless individuals lack updated identity cards or have lost documents during "street cleaning" operations conducted by the government. Without these, the fee waiver process stalls.
- The Comprehensive Social Security Assistance (CSSA) Bottleneck: While CSSA recipients are technically exempt from many fees, many homeless individuals do not or cannot enroll in CSSA due to the lack of a fixed address or the stigma associated with the "dole." The fee hike disproportionately hits the "non-CSSA" homeless—those who may have some intermittent income but fall below the poverty line.
Geographic and Temporal Barriers
The cost of healthcare is not just the fee paid at the window; it is the cost of transit and the "opportunity cost" of waiting.
- Transit Costs: Public hospitals and clinics are not always within walking distance of popular sleeping spots. For someone with zero income, a HK$10 bus fare is a barrier.
- Wait Times: A six-hour wait at a public clinic for a 5-minute consultation is a deterrent. For those struggling with physical mobility or mental health issues, the stamina required to navigate the public system is a resource they do not possess.
Quantifying the Economic Paradox
The logic behind increasing medical fees is often fiscal sustainability—recouping costs to fund the broader system. However, in the context of the homeless, this is a mathematically flawed strategy.
Consider the cost function:
$$Total\ State\ Cost = (C_{primary} \times N) + (C_{emergency} \times P_{failure})$$
Where:
- $C_{primary}$ is the cost of a subsidized clinic visit.
- $N$ is the number of preventative visits.
- $C_{emergency}$ is the cost of an emergency room visit, hospitalization, or surgery.
- $P_{failure}$ is the probability that a skipped visit results in an acute medical crisis.
When $C_{primary}$ increases, $N$ decreases (as seen in the 60% survey figure). This directly increases $P_{failure}$. Because $C_{emergency}$ is orders of magnitude higher than $C_{primary}$, the total state cost actually rises as a direct result of the fee hike. The state is effectively trading a small, manageable expense now for a catastrophic, unmanageable expense later.
The Invisible Attrition of the "Work-Able" Homeless
There is a segment of the homeless population that engages in low-wage, informal labor—collecting cardboard, site cleaning, or delivery work. For this group, the health-fee-work nexus is particularly brutal.
- The Injury-Poverty Trap: Manual labor leads to musculoskeletal injuries. If the cost of treatment is too high, the individual works through the pain, worsening the injury until they are physically incapable of labor.
- Permanent Dependency: Once the "work-able" homeless become physically disabled due to lack of primary care, they move from being temporary users of the system to permanent dependents on the state's welfare and medical resources.
Strategic Realignment of Healthcare Delivery
The data suggests that the current model of "subsidized but fee-bearing" care is failing. A more robust strategy requires a move toward a high-trust, low-friction delivery system that prioritizes long-term fiscal health over short-term fee recovery.
Implementation of Mobile Clinical Units
Instead of requiring the homeless to navigate the bureaucracy of the hospital system, healthcare must be delivered at the point of need. Mobile units that provide basic diagnostics, medication dispensing, and fee-waiver processing on-site eliminate the transit and administrative barriers. This "active case finding" approach ensures that 60% of the population isn't "planning to cut visits" because the visit comes to them.
Decoupling Healthcare from Fixed-Address Documentation
The government must create a "Vulnerable Persons Medical Pass" that bypasses standard documentation requirements. This pass should be granted based on the assessment of social workers or recognized NGOs, allowing for immediate, free access to primary care without the need for CSSA enrollment or proof of residence.
The Fiscal Necessity of Free Primary Care
The most aggressive but logical move is the total elimination of fees for the bottom 5% of the income bracket, specifically for primary care and chronic disease management. While this appears to be a loss of revenue, the resulting reduction in emergency room "revolving door" cases—where the same individuals are admitted repeatedly for preventable crises—would yield a net positive on the public health budget.
The current policy of incremental fee increases is a textbook example of "penny wise, pound foolish" governance. By pricing the most vulnerable out of the preventative system, the state is not saving money; it is financing a future of more expensive, less effective, and more frequent medical emergencies. The strategic path forward is not a refinement of the waiver system, but a radical simplification of access that recognizes health as the primary variable in the equation of social stability and economic recovery.